



Context - Global public health security depends on actions to prevent and respond to threats that endanger the collective health of the global population. Those threats have an impact on economic or political stability, trade, tourism, access to goods and services and, if they occur repeatedly, on demographic stability.
Global public health security covers a wide range of complex and daunting issues, including the health consequences of human behavior, climate change, weather-related events and infectious diseases, as well as natural catastrophes and man-made disasters, all of which are discussed here.
This Digest is a faithful summary of the leading scientific consensus report produced in 2007 by the World Health Organization (WHO): "A safer future: global public health security in the 21st century, 2007![]()
Over the last two centuries, science made huge progress in the fight against infectious disease. But the biggest battles may still be to come:
These and other threats are explored by the World Health Organization, which recommends ways countries can cooperate more closely to protect global public health. More...

Throughout history, humanity has been challenged by devastating outbreaks of infectious diseases. More...
2.1 Separating the sick from the healthy is an ancient approach to disease control, notably for leprosy. The practice became known as “quarantine” in the late 14th century, when people arriving in ports from plague-infected areas were isolated for at least 40 days. Quarantine became commonplace over the following centuries, although it proved to be largely ineffective on its own. More...
2.2 A breakthrough in the understanding of how disease spreads came during the cholera epidemic in London in the mid-19th century, when an British doctor, John Snow, discovered that cholera was transmitted through contaminated water. His discovery led to improvements in water sanitation in industrialized countries that greatly reduced the risk of the disease. Cholera, however, remains a major health risk in developing countries where clean water is lacking. More...
2.3 In the 18th century, another British doctor, Edward Jenner, discovered a vaccine for smallpox, one of the oldest and deadliest of human diseases. In 1979, a global immunization campaign succeeded in eradicating the disease. Small samples of the virus have been kept for research purposes, which raises fears that the virus could reappear as a devastating biological weapon. More...
2.4 The need for international coordination on public health led to the creation of the WHO in 1948. International health regulations were established in 1969 to limit the spread of infectious diseases across international borders.
The regulations were widened and strengthened in 2005 because in today’s highly mobile world, borders cannot stop the spread of diseases, and because new diseases are appearing, and spreading from animals to humans. More...

Many public health threats are due to human action or lack thereof whether deliberate or not. More...
3.1 In the absence of major health threats, governments tend to lower their guard and spend less on public health. For instance, large-scale insecticide spraying campaigns in the 1960s nearly eradicated many diseases carried by insects, but these re-emerged after spraying programmes stopped. More...
3.2 Warfare is another threat to public health – and not just because people die in the fighting. Armed conflict can destroy health care systems, leaving people more vulnerable to infectious disease, especially populations displaced by conflict. For instance, some 50 000 people who fled the ethnic bloodshed in Rwanda in 1994 died of cholera within a month of their arrival at a crowded refugee camp. More...
3.3 The widespread and sometimes incorrect use of antibiotics has favored the emergence of bacteria that no longer respond to standard treatments. This threatens our ability to treat major killers like tuberculosis. More...
3.4 Poor animal feeding and rearing practices can cause disease outbreaks which may then spread from animals to humans. In fact, many new and emerging diseases, such as mad cow disease, originate from animals. More...
3.5 Changes in climatic conditions can modify the geographic spread of infectious diseases. For instance, increased rainfall can put people at a greater risk to be infected by some illnesses carried by insects. More...
3.6 Use of chemicals and reliance on nuclear energy call for public health security measures. There is always a risk of spills, leaks, accidents and deliberate releases which could threaten health. More...
Three events illustrate new health threats of the 21st century: the 2001 anthrax letters in the United States, the emergence of SARS in Asia in 2003, and the illegal dumping of chemical waste in Ivory Coast in 2006. More...
4.1 In 2001, letters containing anthrax spores were mailed to several U.S. media offices and two U.S. senators, killing five people and infecting 17 others. These attacks caused huge alarm and prompted a massive public health response. They showed the potential of bioterrorism to cause social and economic havoc and prompted a profound rethinking of threats to national and international security. More...
4.2 SARS (Severe Acute Respiratory Syndrome) killed hundreds of people and affected thousands during a 2003 epidemic raising the threat of a worldwide epidemic (or “pandemic”). Previously unknown, this pneumonia-like disease is caused by a virus transmitted by close contact with an infected person. Believed to have originated in China, it spread swiftly around the world, apparently passed on by people traveling by plane. It brought travel to affected areas to a standstill and drained billions of dollars from Asian economies. More...
4.3 Not only the international mobility of people, but also the global movement of products can have serious health consequences. In August 2006, a cargo ship traveling from Europe to various African ports illegally unloaded and dumped over 500 tons of chemical waste in Ivory Coast. Tens of thousands of people went to medical centers with health complaints and fears linked to the chemical waste, overwhelming the medical system that was already short-staffed and under-equipped. Sixty-nine people were admitted at the hospital, and at least eight of them died as a result of the incident. More...

Influenza, the infectious disease commonly known as flu, is caused by a virus that mutates frequently. Occasionally a particularly virulent strain of the virus spreads swiftly around the world, affecting or even killing a large proportion of the population. This constitutes a pandemic. The world has suffered several influenza pandemics over the last century including the 1918-1919 “Spanish Flu” that killed millions. More...
5.1 Every year, human influenza rapidly spreads around the world in seasonal epidemics of significantly lesser proportion than pandemics, but still resulting in an estimated three to five million cases of severe illness and as many as 500 000 deaths, mostly amongst the elderly.
For the last 50 years, a global surveillance network has been monitoring the constantly changing influenza viruses, and guiding the preparation of seasonal vaccines. More...
5.2 Avian influenza is an emerging disease, and the current virus causing it, known as H5N1, has decimated wild bird populations in parts of the world and forced the slaughter of millions of domesticated birds. While the virus has caused a number of infections in humans who had close contacts with infected birds, it has not yet mutated into a form that spreads easily from person to person. But authorities are preparing for this possibility. By some predictions, H5N1 could create a pandemic affecting about 1.5 billion people and causing enormous economic and social disruption. More...
5.3 WHO has developed a strategic action plan to help countries prepare for an influenza pandemic and has assisted countries that have experienced outbreaks of human cases of avian influenza. In order to further strengthen the international response, the United Nations System Influenza Coordination (UNSIC) was established in 2005 to respond to government requests for coordinated and sustained international support to implement avian and human influenza programmes. More...

Tuberculosis, caused by airborne bacteria, is a leading killer among infectious diseases. Drug-resistant strains of tuberculosis have emerged, compromising our ability to treat it. Cases of “extensively drug-resistant tuberculosis” have been confirmed in at least 37 countries. Affected patients are unresponsive not only to the standard antibiotic treatment, but also to several new stronger antibiotics, and drug resistant tuberculosis may be as contagious as treatable strains.
While bacteria can naturally develop resistance to antibiotics, “extensively drug-resistant tuberculosis” generally develops as a result of patients not fully following the prescribed treatment. This can be due to poor supervision, both of the patient and the medical staff, disruptions in drug supplies and poor clinical management.
Because AIDS weakens the immune system, its spread has contributed significantly to the resurgence of tuberculosis as a major public health threat. The concentration of HIV-infected people in hospitals exacerbates the risk of catching tuberculosis. In patients infected with HIV, untreated tuberculosis will cause death in weeks. More...
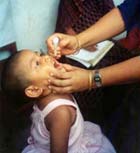
Poliomyelitis, often called polio, is a viral disease attacking the nervous system, which can lead to paralysis. By the end of the 20th century, vaccinations and close monitoring had nearly succeeded in eradicating it. However, in 2003, Nigeria stopped vaccinating children in parts of the country because of unsubstantiated claims that the oral vaccine was unsafe, giving rise to a large polio outbreak. It left thousands of children in Nigeria paralyzed and spread to countries in Africa, Asia and the Middle East. Under international pressure, Nigeria resumed vaccination the following year but the epidemic continued until 2006.
Today polio cases are once again declining but the Nigerian experience is a reminder of the need to remain alert and ready to respond to any outbreak or mutation of the virus. These efforts must continue after polio is eradicated in the wild, in case samples of the virus preserved for research are accidentally or deliberately released. More...
8.1 It is necessary that all countries have a robust health system to ensure an unbroken line of defense against infectious diseases. Developing countries, however, are struggling to provide basic health care to their populations.
Besides strong health care, more cooperation between countries, international organizations and different sectors of society would help prevent public health emergencies from becoming international threats. More...
8.2 To achieve the highest possible level of global public health security, WHO recommends:

This summary is free and ad-free, as is all of our content. You can help us remain free and independant as well as to develop new ways to communicate science by becoming a Patron!