

Langues:

Resistance is a natural phenomenon. Bacteria adapt to their environment and have mechanisms to pass on genetic information across species. It is inevitable that resistance to any antibiotic will develop at some time. As misuse and overuse of antibiotics accelerate the development of resistance, antibiotics should be used more responsibly and new antibacterial treatments should be developed to counteract emerging resistance.
The emergence and spread of antibacterial resistance in all geographical areas, including in bacteria that cause hospital- and community-acquired infections, is jeopardizing the effectiveness of life-saving treatments. The threat includes the spread of multidrug-resistant bacteria, and infections with no therapeutic options have been reported.
Since the 1980s, the total number of new antibiotics approved has fallen significantly, increasing only slightly between 2011 and 2016.
The rise in resistance not only impedes the ability to treat bacterial infections in humans and animals but has broader societal and economic effects that ultimately threaten achievement of the Sustainable Development Goals1. This situation requires urgent, coordinated action at global, regional and national levels.
1
http://www.un.org/sustainabledevelopment/sustainable-development-goals/![]()
WHO drew up a list of priority antibiotic-resistant pathogens to guide research into and the discovery and development of new antibiotics. Tuberculosis (TB) is the number one global infectious disease killer today, causing 1.8 million deaths per year. Drug-resistant TB is the most common and lethal airborne antimicrobial-resistant disease worldwide today, responsible for 250 000 deaths each year. Only two new antibiotics for treatment of Multi-drug-resistant-TB have reached the market in over 70 years. Research and development (R&D) investment in TB is seriously underfunded, and at its lowest level since 2008.
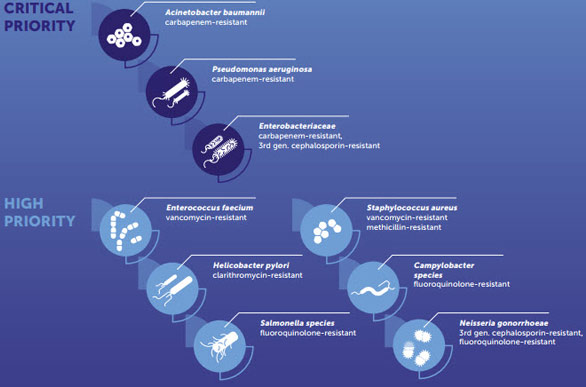
The other pathogens of critical priority are those that are resistant to carbapenem, a drug used for the treatment of resistant infections, which is administered intravenously in hospital settings.
As part of implementation of the Global Action Plan on Antimicrobial Resistance adopted in 2015, WHO Member States committed themselves to prepare national action plans and, among other things, to promote the development of new antibiotics.
Recent initiatives have started, and in 2016 more than 90 pharmaceutical, diagnostics and biotechnology companies and industry associations from different countries committed to engage in collaborative initiatives with academia and public bodies to enhance antibiotic discovery, and agreed on a roadmap to reach this aim.
More innovative products are required against pathogens with no cross- or co-resistance to existing classes but the WHO review shows that the current clinical pipeline is still insufficient to mitigate the threat of antimicrobial resistance. This is because there is a lack of potential treatment options for priority resistant bacteria, especially for multidrug- and extensively drug-resistant Gram-negative pathogens. Also, although oral formulations for community diseases associated with high morbidity are essential, few oral antibiotics for infections caused by Gram-negative2 pathogens are in the pipeline.
The two main reasons are that:
2 The gram-negative bacteria include the model
organism![]()
![]()
![]()
As of May 2017, 33 antibiotics and 9 biological agents including monoclonal antibodies and endolysins (a class of enzymes derived from viruses that attack bacteria) that target priority pathogens were in the clinical pipeline with seven products for tuberculosis (TB) and nine for C. difficile infections. Among the 33 antibiotics, eight belong to five distinct new antibiotic classes, and they fulfil at least one of the four criteria that were used to assess the extent to which agents in the pipeline can be classified as innovative:
Marketing approval of new antibiotic classes (16 products in the current pipeline) has increased therapeutic options for multidrug-resistant Gram-positive pathogens, specifically methicillin resistant Staphylococcus aureus, but new treatments for those pathogens are still required to keep up with the anticipated evolution of resistance. Another highly important pathogen, vancomycin-resistant Enterococcus spp., has received little attention and the situation is worse for Gram-negative bacterial infections emerging worldwide and that cannot be treated with any of the antibiotics currently on the market. Almost all the agents are modifications of existing antibiotic classes and address specific resistance mechanisms. They are active only against specific pathogens or a limited subset of resistant strains.
Only seven new agents that target tuberculosis are currently in clinical trials and only one compound is in clinical development phase-3. This is especially problematic because treatment of TB infections requires a combination of at least three antibiotics. Novel treatment regimens of short duration that are assembling non-toxic drugs are desperately needed.
The likelihood of future approvals of antibiotics that are in clinical development phase-1 has been estimated to be 14% and the current pipeline of antibiotics and biologicals could lead to around 10 new approvals over the next five years but adding little to the already existing arsenal and will not be sufficient to tackle the impending antibiotic resistance threat.
There are also two types of new approaches referred to as “biological treatments” that are being looked at to complement antibiotics. Whether so called biological treatments could serve as real alternatives to antibiotics is not yet clear and their higher costs may also limit their potential use as alternative treatments especially in low and middle income countries.
Contribution of the pharmaceutical industry remains a key success factor and essential in bringing new therapeutic products to the market. But presently universities and other publicly funded research institutions are often the source of the technology that is the starting point for R&D projects in small and medium-sized enterprises. Many of these products are already co-funded by research grants from public and philanthropic institutions. Especially for tuberculosis, most development is undertaken by not-for-profit entities.
The development of new antibiotics should go hand in hand with infection prevention and control activities, as well as fostering of appropriate use of existing and future antibiotics through stewardship measures. The WHO Global Development and Stewardship Framework to Combat Antimicrobial Resistance should in particular provide the necessary guidance for using antibiotics more responsibly in the human, animal and agricultural sectors.
In this context the WHO regularly updates its guidelines on appropriate prescribing of antibiotics : How to stop antibiotic resistance? Here's a WHO prescription3.
3 How to stop antibiotic resistance? Here's a WHO prescription
http://www.who.int/mediacentre/commentaries/stop-antibiotic-resistance/en/![]()

This summary is free and ad-free, as is all of our content. You can help us remain free and independant as well as to develop new ways to communicate science by becoming a Patron!